Polypectomy
Polypectomy is a minimally invasive procedure in which healthcare providers remove abnormal growths of tissue, called polyps, from inside your colon. In addition to being part of a routine colonoscopy and a therapeutic procedure, a polypectomy is used as a means to assess whether a growth is cancerous, precancerous, or noncancerous.
You may need a polypectomy if you have a polyp inside your colon, which can be discovered during a colonoscopy—a routine exam recommended for adults 45 years of age or older to check for any growths that may indicate cancer. A polyp may also be detected during a non-invasive imaging test, such as a computed tomography (CT) scan, ultrasound, or a magnetic resonance imaging (MRI) scan when you are being evaluated for weight loss, bleeding, or other symptoms.
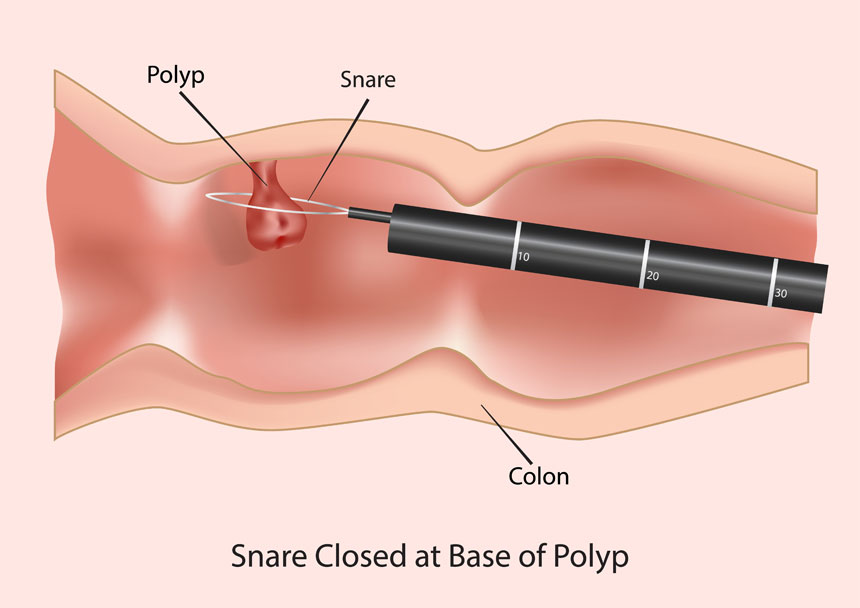
A polypectomy is performed whenever a polyp that needs to be removed is found, and the procedure is usually done during the very colonoscopy that reveals one. A polyp remaining inside the colon can bleed, grow, or become cancerous.Often, when a polyp is removed, it is examined under a microscope like a biopsy, so that you and doctor will know if it was cancerous and whether there is any evidence that any remaining tissue also needs removal.
A polypectomy can cause bleeding, a perforation, or an infection. If you need a polypectomy and take blood thinner, it is almost always recommended to discontinue them prior to the procedure.If you have an infection of your gastrointestinal system, a polypectomy can trigger the spread of infection, so it is likely that doctor will want you to wait until after the infection has resolved before you have the procedure.
A perforation, in which the bowel is cut, is a rare complication of polypectomy. If this happens, you will need emergency surgery to repair the lacerated colon.
